Persistent heartburn or reflux may be more than just a dietary issue — it could be a sign of a hiatal hernia. At the Hernia Institute of Louisiana in Metairie, Dr. David C. Treen, Jr., a Fellow of the American College of Surgeons, specializes in diagnosing and treating hiatal hernias. He and his team help patients find lasting relief when lifestyle changes and medications aren’t enough.
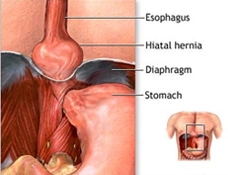
What Is a Hiatal Hernia?
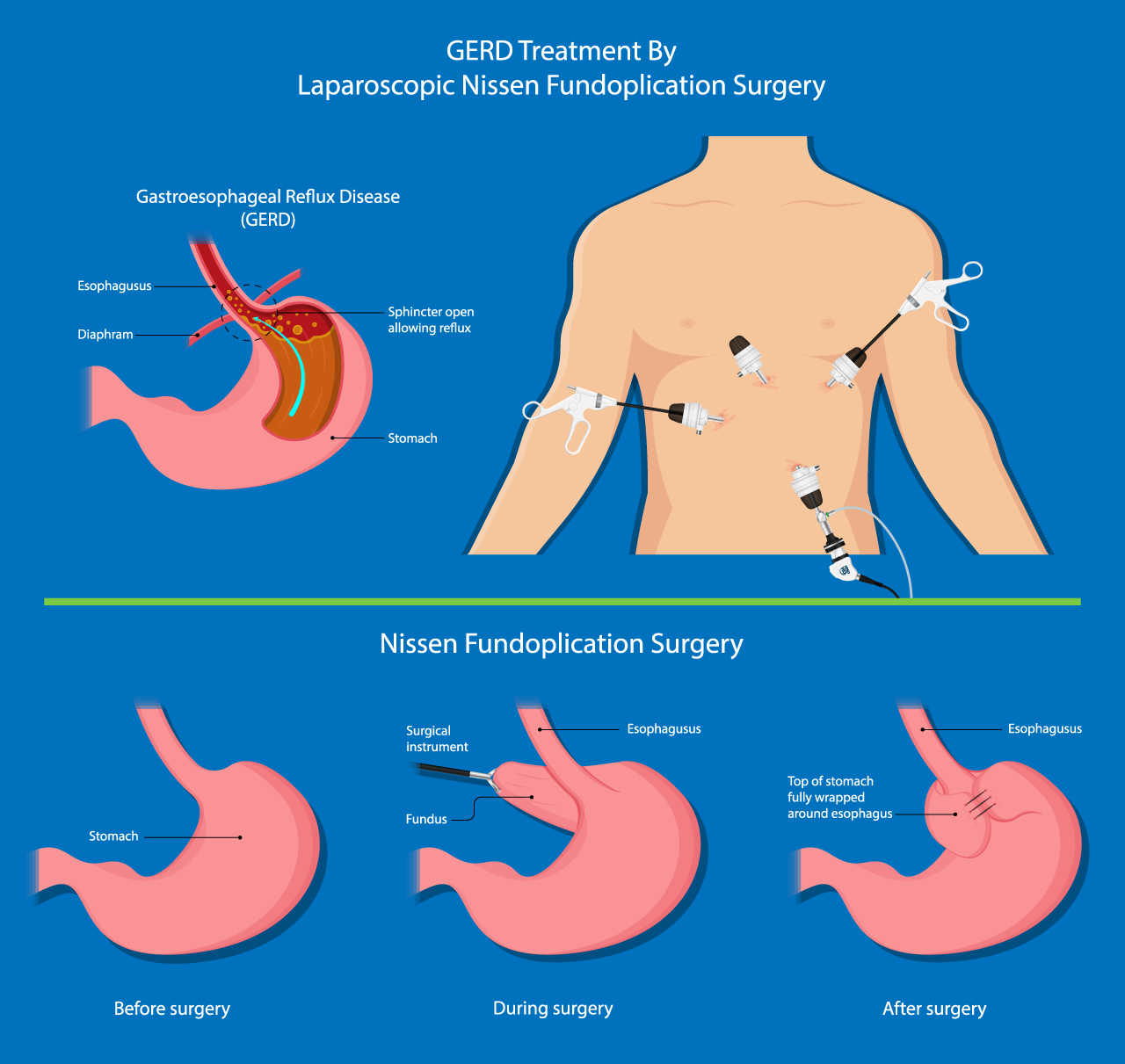
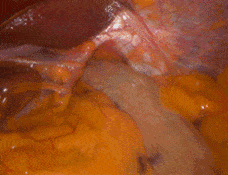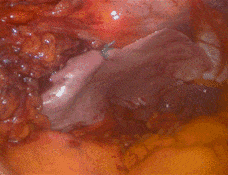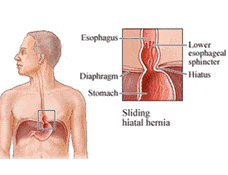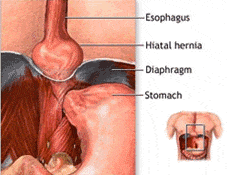
A hiatal hernia occurs when the upper part of the stomach pushes through the diaphragm into the chest cavity through a widened esophageal opening (hiatus). This opening, normally teardrop-shaped, can become dilated, allowing stomach contents to move upward, often causing or worsening symptoms of gastroesophageal reflux disease (GERD).
Hiatal hernias vary in severity. In some cases, they cause mild reflux; in others, they contribute to chronic GERD that doesn’t respond to conservative treatment.
Common Symptoms
Signs of a hiatal hernia include:
- Frequent heartburn
- Regurgitation of food or sour liquid
- Difficulty swallowing
- Chest discomfort or pressure
- Worsening reflux symptoms when lying down or bending over
Hiatal Hernia Causes
Several factors can contribute to the development of a hiatal hernia:
- Age-related changes in the diaphragm
- Increased abdominal pressure from obesity, heavy lifting, persistent coughing, frequent vomiting, or straining during bowel movements
- Pregnancy
- Genetics (some people are born with a naturally larger hiatus)
Types of Hiatal Hernias
A sliding hiatal hernia occurs when the stomach and lower portion of the esophagus slide upward through the hiatus into the chest. This type is frequently associated with GERD symptoms.
A paraesophageal hiatal hernia is less common but more complex. In this case, the stomach pushes through the opening and sits next to the esophagus rather than sliding with it.
Larger or mixed hernias can involve multiple portions of the stomach moving into the chest cavity, which may require surgical treatment.

Diagnosing Hiatal Hernias
Diagnosing a hiatal hernia typically involves a combination of medical history, symptom evaluation, and specialized testing.
A physician may begin by reviewing symptoms such as persistent reflux, chest discomfort, or swallowing difficulties. Imaging tests are commonly used to confirm the diagnosis and evaluate the anatomy of the esophagus and stomach.
A barium swallow study can highlight how food moves through the digestive tract and reveal a hernia. An upper endoscopy also allows the physician to visually examine the esophagus and stomach using a small camera.
Additional testing, such as esophageal manometry or pH monitoring, may be recommended in certain cases.
Surgical Treatment for Hiatal Hernias
Hiatal hernia repair is typically performed laparoscopically under general anesthesia. The procedure involves reducing the hernia, tightening the diaphragm’s opening, and reinforcing the area to prevent recurrence. Most patients only require an overnight hospital stay and can return to normal activities in 5–10 days.
A major concern with traditional repairs is a high recurrence rate — studies suggest that repairs without mesh can result in recurrence in up to 25–30% of cases. While not all recurrences cause symptoms, they may eventually require revision surgery.
Advanced Mesh Options
Historically, synthetic mesh in hiatal hernia repair has been associated with complications, including erosion or scarring around the esophagus. That’s why our team uses biologic mesh when reinforcement is necessary. These biologically derived materials integrate more naturally with the body, significantly reducing the risk of mesh-related complications.
The Device: A Modern Option for GERD
For select patients with chronic reflux, the device may offer an innovative alternative to traditional repair. This small bracelet of magnetic beads is placed around the esophagus just above the stomach. It opens to allow food through and closes to prevent acid reflux.
The device:
- Is minimally invasive
- Is typically inserted as an outpatient procedure
- Allows most patients to return to daily activities quickly
Why Choose the Hernia Institute of Louisiana for Hiatal Hernia Repair in New Orleans, LA?
Dr. Treen brings more than 20 years of experience in advanced surgical care, with leadership roles in national organizations and academic medicine. He is committed to providing customized treatment options for every patient based on anatomical complexity, symptom severity, and long-term outcomes.
Our advantages include:
- Expert laparoscopic surgical team
- Use of biologic mesh for safer, more effective repairs
- Access to the device when appropriate
- Personalized care focused on lasting relief
FAQs
Are There Non-Surgical Treatments That Can Help Manage a Hiatal Hernia?
Many people manage mild hiatal hernia symptoms with lifestyle adjustments such as eating smaller meals, avoiding trigger foods, maintaining a healthy weight, and not lying down soon after eating. Elevating the head of the bed can also help limit nighttime reflux. Medications like proton pump inhibitors, H2 blockers, and antacids are commonly used as well.
While these approaches can control symptoms for many patients, they do not repair the hernia itself. When symptoms persist or complications develop, surgical treatment may be recommended.
Can a Hiatal Hernia Cause Breathing Problems or Chronic Cough?
In some cases, a hiatal hernia can contribute to breathing difficulties or a persistent cough. When stomach acid frequently moves into the esophagus, it can irritate the throat and airway, sometimes triggering coughing or a sensation of shortness of breath. Reflux-related irritation may also worsen asthma symptoms in certain individuals.
Large hiatal hernias may compress nearby chest structures, contributing to chest discomfort or breathing changes. Chronic coughing caused by reflux can further aggravate the hernia by increasing abdominal pressure. Treating the underlying reflux or repairing the hernia may help reduce these respiratory-related symptoms.
What Is the Difference Between Hiatal Hernia Repair and Fundoplication?
Hiatal hernia repair and fundoplication are related procedures, but they serve slightly different purposes.
- Hiatal hernia repair focuses on correcting the anatomical problem by pulling the stomach back into the abdomen and tightening the opening in the diaphragm (the hiatus) to keep the stomach from moving upward again.
- Fundoplication is a technique used to control acid reflux. During this procedure, the upper part of the stomach is wrapped around the lower esophagus to strengthen the valve that prevents stomach acid from flowing backward.
In some cases, both procedures are performed together to address the hernia and reduce reflux symptoms.
Schedule Your Hiatal Hernia Consultation
If you’ve been battling GERD or suspect a hiatal hernia, the Hernia Institute of Louisiana is here to help. Schedule a consultation with Dr. Treen to explore your treatment options. Call 504-218-4922 today and take the first step toward greater comfort.